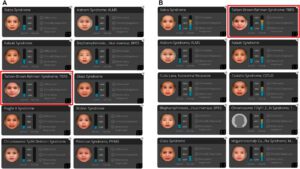
After a successful experience using Face2Gene in his telehealth clinic in Scottsbluff, Dr. Abdul-Rahman decided to start another clinic using the same model, this time even further away in Gordon, Nebraska.
WHO
Dr. Omar Abdul-Rahman is the Director of Genetics at the Munroe-Meyer Institute.
THE DILEMMA
Here, they saw a young child, only a few months old, with non-specific syndromes, including developmental delay and low muscle tone.
THE SOLUTION
He had no specific syndrome in mind for the patient, and Face2Gene gave a pretty broad differential, so he ordered a microarray analysis. A couple of weeks later, he received results showing that the patient had a microdeletion in the Prader-Willi/Angelman syndrome critical region. Though these syndromes present differently, they may be hard to differentiate at a very young age. Reviewing his clinical notes, he found nothing to really pinpoint the diagnosis one way or another, but he did see that Angelman was one of the highly ranked syndromes in Face2Gene, and Prader-Will was not on the list of highly ranked results. When the family returned to the telehealth clinic months later, he saw further clinical signs to support the diagnosis of Angelman syndrome.
THE RESULT
Although the family’s insurance refused to cover confirmatory testing, Dr. Abdul-Rahman felt confident in making a clinical diagnosis of Angelman syndrome, backed up by the results of the patient’s Face2Gene analysis.
“Now we’re talking to our faculty about more telehealth clinics, and to me, this is the model that works,” said Dr. Abdul-Rahman. “We can interact with the patient. We can talk with them and get a history. But when it comes to the physical exam, using Face2Gene as an adjunct tool is really critical.”
Though the use of Face2Gene in telehealth clinics is an approach unique to Dr. Abdul-Rahman’s genetics team, the challenges they are facing are not unique. This novel telehealth approach could have a great impact on many patients and families in remote areas.