Note: This talk was presented at the 2018 ACMG annual meeting. The video can be seen below, or at this link>
HISTORY
Since the 1960s, the field of medical genetics has been evolving rapidly with regard to phenotype delineation and analysis.
A disease phenotype requires a multi-faceted analysis. Besides defining the phenotype with diagnostic criteria, medical geneticists are also faced with the challenge of drawing lines along spectra of manifestations and within disease definitions, allowing for how symptoms may change over time.
To measure these variables, biochemical analysis, detailed histories, anthropometrics, standardized measures and medical imaging can be applied in concert. As next-generation sequencing evolves the way the medical field examines patients’ genomes, next-generation phenotyping integrates these changes into the analysis of human health, maximizing the impact of new sequencing technologies.
“We’ve actually entered a new golden era of phenotyping,” Dr. Carey said.
PHENOTYPIC DOMAINS
Dr. Carey noted there are three domains to measure disease: diagnostic criteria (a.k.a. definition of the phenotype), the spectrum of manifestations and complications, and natural history how the phenotype changes over time.
SYNDROME DELINEATION
Syndrome delineation has three distinct parts, as Dr. Carey reviewed in Charlotte, N.C. The first, the physical examination, involves observations and descriptions of the patients. Then there are two levels of syndrome genesis to consider: formal (e.g., a shortage or malformation of a critical enzyme) and causal (e.g., the genetic source of the formal genesis, such as a deletion or de novo mutation.)
SYNDROME GROUPS & HETEROGENEITY
The broad definition of syndrome classification is misleadingly simple: simply group patterns of anomalies, with at least one being morphologic, thought to be etiologically related. Of course, in practice, this is very different than in theory; groups of syndromes, variant forms, subtypes or related disorders can be hard to separate into discrete syndromes. Similar phenotypes can be caused by errors in different genes, or by multiple genes, and identical mutations can cause different phenotypes across patients.
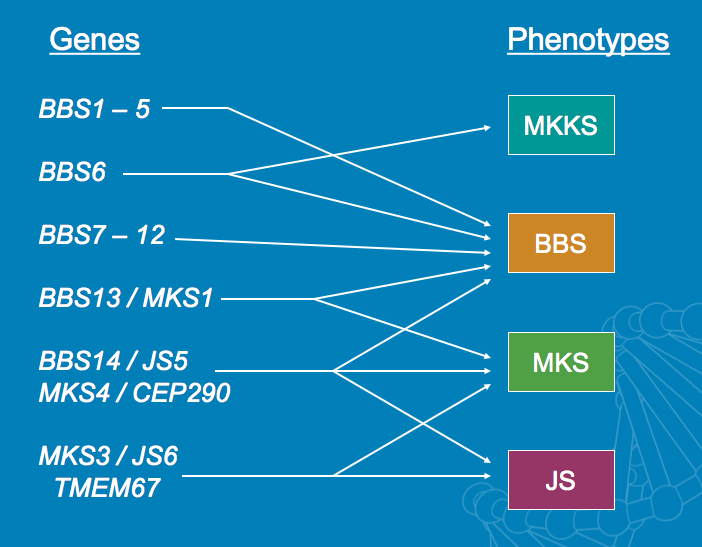
“There are syndromes we know quite well that have 17 genes. There’s one gene that has 17 syndromes. Do we go with the gene or do we go with the phenotype?” Dr. Carey asked the audience.
THE AXIS MODEL
To solve these discrepancies, Dr. Carey proposed the use of the “axis model.” Axis I describes the clinical phenotype, Axis II describes the underlying molecular genetics, and Axis III describes non-genetic factors, like the environment.
“It’s never been adapted but I actually like it,” he said.
I would propose that even though you can’t [describe a syndrome in] 3 or 4 words, or less, Dr. Carey said of the sometimes wordy model. Despite its potential complication, its focus on phenotype keeps the naming mechanism patient-centered.
Watch the recording of the talk here.
